Healthcare has changed throughout the years, and continues to be an evolving industry. Nursing models play a vital role in ensuring the best health outcomes for patients, no matter how quickly the industry changes. These models provide a framework for organizing and delivering care, while still considering aspects such as patient needs, staffing levels and resource availability. In this article, we will look at the nursing models that are commonly used in delivering this care, and their impact on patient outcomes.
Table of Contents
Individual nursing
The individual nursing model is designed to address the unique needs of each patient. It recognizes that no two people are exactly alike, even if they have the same or a very similar diagnosis. By taking standardized care plans and adapting them to the specific patient, healthcare professionals can provide personalized care based on a wide range of factors.
One of the key aspects of individual nursing is the emphasis on patient-centered care. This means that whenever possible, care plans will be based on the patient’s preferences, values and cultural background. Involving patients in their own care decisions creates a collaboration between healthcare professionals and patients.
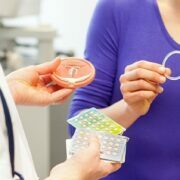
One example of the impact that the individual nursing model has on patient outcomes could be a patient who has been diagnosed with diabetes. Rather than offering a one-size-fits-all care plan, the individual nursing model would factor in specifics, such as their age, lifestyle and any other illnesses they have. The nurse would work closely with the patient to develop a personalized care plan that aligns with their needs and preferences. This can include education on managing their condition, such as dietary modifications tailored to their food preferences and cultural practices. The nurse would also provide guidance on carbohydrate counting, portion control and meal planning, considering the patient’s specific dietary restrictions or preferences, if the diagnosis was linked to or worsened by specific foods and drinks. With diabetes, this is often the case. As most foods contain sugar, it’s challenging for those who are newly diagnosed to find a suitable diet that works for them.
Additionally, the nurse would collaborate with the patient to determine the most suitable method for administering insulin, whether it is through injections, an insulin pump or another delivery system. They would provide detailed instructions and hands-on training to ensure that the patient feels confident and empowered to manage their condition effectively. Self-injection can be daunting at first and other options may be sought for anyone who continues to struggle with this.
Personalizing the care provided increases patient satisfaction. It’s impossible to constantly monitor patients, so it’s important to find a plan they are comfortable with. Patients feel valued and heard as their unique needs are taken into account. This leads to improved health outcomes.
When patients actively participate in their care and feel empowered to make informed decisions, they are more likely to adhere to treatment plans, follow recommended lifestyle modifications, and manage their condition effectively. This can result in better glycemic control, reduced risk of complications and an overall improvement in their quality of life.
The individual nursing model allows for ongoing assessment and adjustment of the care plan as needed. As the patient’s condition either improves or deteriorates, the nurse can modify the care plan but make sure that it still aligns with the patient’s changing and unique needs.
The use of specialized nursing tools and ongoing education, through courses such as those offered by Spring Arbor University, also play a crucial role in ensuring the best health outcomes for patients. Tools such as electronic health records and clinical decision support systems assist nurses in documenting patient information, tracking medication administration and accessing evidence-based guidelines. These tools streamline workflows, reduce errors, and enable nurses to make informed decisions based on the latest research and best practices.
Continuous education is essential for nurses to stay updated with advancements in healthcare, use the tools efficiently, and enhance their skills. As the field of healthcare evolves, nurses can pursue further education through reputable institutions such as Spring Arbor University, which offers online programs catering to the needs of working professionals. These programs provide nurses, or those interested in changing careers, with the opportunity to expand their knowledge, develop specialized expertise, and gain advanced degrees that can lead to enhanced career opportunities and improved patient outcomes.
Primary care nursing
The primary care nursing model revolves around assigning a designated nurse to take overall responsibility for the care of one or more patients through every stage of their healthcare journey, from admission to discharge. While this primary nurse will collaborate with other nurses, they play a central role in coordinating services, making important decisions and supervising the overall care.
Two key benefits of the primary care nursing model are continuity and coordination of care. By having a designated nurse whose involvement in the patient’s care is constant, a strong relationship is developed between the nurse, patient and their family. This continuity leads to a deeper understanding of the patient’s needs, preferences and medical history. The primary nurse becomes familiar with the patient’s circumstances and can provide tailored care to address these needs.
Acting as a central point of contact, the primary nurse makes it possible to communicate more effectively, and collaborate with the various healthcare team members involved in the patient’s care. They serve as an advocate for the patient, ensuring that their needs are communicated and addressed as much as possible. This comprehensive approach minimizes the risk of fragmented care and improves patient safety by reducing the potential for miscommunication or gaps in information.
The primary care nurse coordinates and oversees the delivery of care, ensuring that all aspects of the patient’s treatment plan are implemented effectively. It’s impossible for any nurse to be physically present for the patient all the time. However, they actively engage in care planning, using their expertise and knowledge to make the best decisions about their patient’s care. This includes monitoring the patient’s condition, administering medications, coordinating diagnostic tests and procedures, and providing emotional support. Generally, they will be informed of any relevant information about their patient.
The primary nurse ensures that this information is effectively communicated during handoffs, both within the healthcare facility and when transferring the patient to another facility or home care. This continuity of care reduces the risk of errors or omissions and enhances patient safety during these critical transitions.
The continuity and coordination of care enables the primary nurse to develop a deeper understanding of the patient’s needs and tailor their care accordingly. Patients are more likely to feel that they are being listened to and supported throughout their healthcare journey.
Functional nursing
The functional nursing model is efficient in some ways, but has limitations that can impact patient outcomes. Tasks are divided among nursing staff based on their specific skills and competencies, with each nurse responsible for a particular aspect of care. For instance, one nurse may handle medication administration, while another focuses on wound care.
The main advantage of the functional nursing model is its ability to allocate limited nursing resources effectively, particularly in settings with a shortage of staff or a high number of patients. By distributing tasks among multiple nurses, it ensures that each staff member can use their expertise and strengths in specific areas, maximizing efficiency and workflow, and reducing errors, which is always a good thing.
However, the functional nursing model has faced criticism for potentially compromising the quality of care and patient outcomes. The fragmented nature of this model means that there is a risk of reduced personalization and a lack of holistic understanding of the patient’s needs. When different nurses are responsible for different aspects of care, it can lead to a disjointed patient experience, as the patient interacts with multiple caregivers instead of having a consistent point of contact.
These challenges can be overcome to some extent with effective communication and coordination among team members, and some of the nursing tools mentioned earlier in this article. This is why accurate and up-to-date records are so important. Nurses need to actively collaborate, share information and ensure a seamless handoff of responsibilities to maintain continuity in care. Regular team meetings, care conferences and open lines of communication can help address any potential gaps or misunderstandings that may arise from the functional nursing model.
It can work if team members are able to develop a complete understanding of the patient’s condition, treatment plan and progress. Electronic health records and other technological tools help in this information sharing and with enhancing coordination among healthcare providers.
While the functional nursing model may offer efficiency in resource allocation, it is important to strike a balance between efficiency and personalized care. Efforts should be made to address the potential limitations of this model by encouraging a culture of collaboration, effective communication and shared responsibility.
Team nursing
The team nursing model combines elements of both primary care nursing and functional nursing, offering a unique approach to care delivery. Tasks are delegated to the relevant clinicians and support staff, while a nurse team leader oversees this delegation and supervision of care.
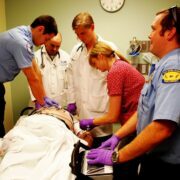
One of the main benefits of the team nursing model is its emphasis on collaboration and shared decision-making among team members. By involving professionals from various disciplines, such as nurses, doctors, therapists and support staff, the model promotes a multidisciplinary approach to patient care. This collaboration allows for a holistic assessment of the patient’s needs and enables a comprehensive treatment plan.
Team nursing also offers flexibility in resource allocation, which was particularly valuable during the COVID-19 pandemic. As patient needs fluctuate, the team nursing model allows for the efficient redistribution of resources and staff members to areas with higher demand. This flexibility ensures that patients receive timely and appropriate care, even during times of increased pressure on healthcare systems.
The team nursing model provides an opportunity for professional growth and skill development among team members. Nurses can learn from each other’s expertise, expand their knowledge base, and enhance their clinical skills through collaboration and shared experiences. Continuous learning and professional development are actively encouraged in healthcare because they contribute to the overall quality of care provided to patients.
It’s important to note that effective delegation and clear communication are crucial in the team nursing model. These ensure that all team members work together cohesively. The nurse team leader plays a vital role in overseeing the delegation of tasks and ensuring that each member understands their responsibilities. Clear communication channels among team members are essential to avoid misunderstandings, ensure patient safety and promote a positive working environment for everyone.
There are some differences between the team nursing model and the functional nursing model. While the functional nursing model assigns specific tasks to different nursing staff based on their skills, the team nursing model encourages a more collaborative and flexible approach. In team nursing, tasks are delegated based on the needs of the patient and the expertise of the team members, allowing for shared decision-making and a broader range of skills to be used in the care provided.
Team nursing also places a greater emphasis on the role of the nurse team leader in coordinating and supervising care, ensuring that all tasks are performed effectively and efficiently. This team leader acts as a central point of contact, facilitating communication and collaboration among team members.
Conclusion
While these nursing models offer different approaches to care delivery, it is important to note that they are not mutually exclusive. Healthcare organizations often employ a combination of these models based on the needs of their patients and the available resources. Ongoing evaluation and quality improvement efforts are essential to ensure that these models are effectively implemented and continuously improved to achieve the best health outcomes for patients.








Comments